How to Deal With a Latex Allergy
Daniel More, MD, is a board-certified allergist and clinical immunologist with a background in internal medicine.
Learn about our editorial processUpdated on March 08, 2022Medically reviewedVerywell Health articles are reviewed by board-certified physicians and healthcare professionals. Medical Reviewers confirm the content is thorough and accurate, reflecting the latest evidence-based research. Content is reviewed before publication and upon substantial updates. Learn more.byJohn Carew, MD Medically reviewed byJohn Carew, MDJohn Carew, MD, is board-certified in otolaryngology and is an adjunct assistant professor at New York University Medical Center.
Learn about our Medical Review BoardTable of ContentsView AllTable of ContentsLatex is the major ingredient in most rubber products and is made from the tree Hevea brasiliensis. Thousands of household and occupational products contain latex, from shoes to rubber bands. This material is especially common in the healthcare industry, where it can be found in surgical gloves and various pieces of medical equipment.
There is much confusion surrounding the topic of latex allergies and there are two distinct types of allergic reactions. First, latex is not the same as many synthetic rubber materials, such as butyl or petroleum-based synthetic products. Paints that are labeled “latex-based” contain a synthetic product that has not been shown to cause problems for people with latex allergies.
Overview
The tendency to develop allergies is inherited. As with other allergies, the more intense and frequent the exposure to latex, the more likely a person will develop an allergic reaction. Between five and 10 percent of healthcare workers develop latex allergies as a result of repeated exposure to latex-containing products. The decreased use of powdered latex gloves (most latex gloves are now non-powdered) seems to have lowered the occurrence of latex allergies in healthcare professionals.
Other groups at risk for latex allergy include those who have had various surgeries, especially those involving the nervous system and genitourinary tract system. Children with spina bifida appear to have a high occurrence of latex allergy.
Symptoms
In general, there are two types of allergic reactions to latex: Immediate and delayed.
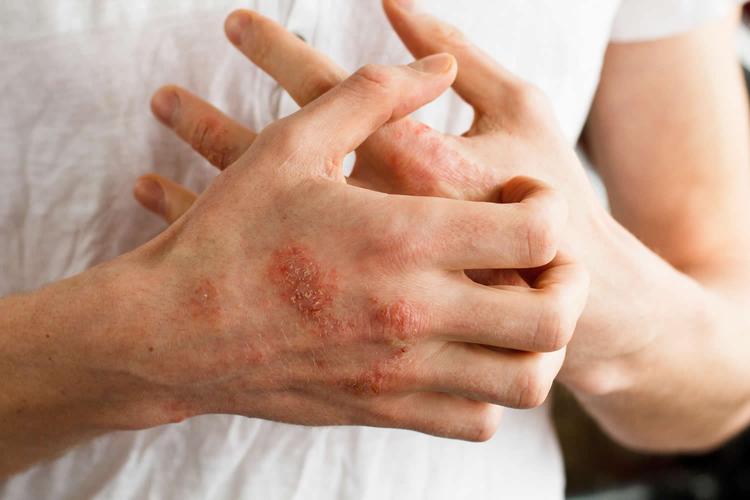
Delayed reactions to latex include itchy, red and mildly swollen rashes that appear only at the sites of contact with the latex product. These rashes typically appear within 12 to 48 hours after exposure and are not life-threatening. This kind of reaction is similar to one caused by poison oak (contact dermatitis) and is due to other chemicals used in the making of latex, rather than the latex protein itself.
An immediate reaction latex allergy, on the other hand, is a potentially serious reaction that occurs within minutes of exposure and may cause hives, itching at the site of contact or all over, tightness of the throat, wheezing, difficulty in breathing, anaphylaxis, and even death. Most people may experience these reactions only upon contact with the latex product. Others are so sensitive that they may have a reaction after being given a drug stored in a bottle with a latex stopper or after breathing the powder that comes off latex surgical gloves.
Diagnosis
People who have a delayed allergic reaction to latex often do not have the allergic antibody (IgE) against latex, but can be diagnosed with the use of a patch test. This involves placing other components of the latex (not the latex protein itself) on the skin for approximately 48 hours and interpreting the results of the test at 48 to 96 hours. This test should only be performed by a healthcare provider experienced in the diagnosis of allergies.
However, an immediate latex allergy is due to the presence of IgE against latex and diagnosed with the use of skin testing or RAST. Skin testing for latex may be difficult since there is no commercial latex extract available for skin testing in the United States. Some allergists make their own extract, and many others rely on the RAST for making a diagnosis of latex allergy. These tests should only be performed by a healthcare provider experienced in the diagnosis of allergies.
Association With Oral Allergy Syndrome
Many people with an immediate latex allergy will also have what's called oral allergy syndrome. This is a condition in which a latex-allergic person notices itching and swelling of the mouth after eating certain foods, most commonly banana, melons, avocado, kiwi, and chestnuts. This is due to the presence of proteins in the foods that are similar to those found in the latex. Not all people with latex allergy to react to any or all of these foods.
While most oral allergy symptoms are mild and last only a few minutes, some people can experience more severe reactions to these foods. It is best for a person with latex allergy to avoid any food that causes oral allergy syndrome symptoms.
Prevention and Treatment
The best way to prevent allergic reactions is to avoid exposure to latex. However, latex is extremely common, so it will be difficult to avoid entirely. Inform your healthcare provider and dentist that you are latex allergic, so they will use non-latex gloves and other latex-free medical supplies during office visits.
Household latex can be found in latex balloons, dishwashing gloves, and in latex condoms. These items are known to commonly cause reactions in latex-allergic people. Items less likely (but still possible) to cause a reaction include rubber bands, erasers, rubber toys, elastic in clothing and baby nipples and pacifiers. Read the labels on any rubber product before purchase, and avoid using any of these that contain latex.
Any person with latex allergy undergoing surgery needs to carefully coordinate the procedure with the hospital, surgeons, anesthesiologists, and other medical personnel to ensure that no latex is used during the procedure. This often means that a latex-allergic person is the first surgery of the day, to ensure the operating room is thoroughly cleaned the night before, and that there is no latex contamination from surgeries earlier in the day.
Allergy shots, or immunotherapy, to latex has been tried to prevent reactions with latex exposure, although with mixed results. Another therapy, omalizumab (Xolair®), an injectable anti-allergic antibody used for the treatment of severe asthma, has been tried to prevent a reaction in people suffering from severe latex allergy.
Treatment of immediate reactions after exposure to latex is similar to the treatment for anaphylaxis. This may include the use of injectable epinephrine, corticosteroids, and antihistamines. Treatment of delayed reactions typically only requires topical corticosteroid creams, or in severe cases, corticosteroid pills or syrup.
All patients with a latex allergy should carry injectable epinephrine, either in the form of an Adrenaclick®, Auvi-q, Epi-pen®, or Twinject®, for use if a reaction should occur.
People with a latex allergy should consider wearing a medical bracelet containing their allergy information, including latex allergy, in case of emergencies in which the person cannot communicate. This is extremely important so that emergency medical personnel will know not to use latex-containing materials when caring for the person.
A useful resource for latex-allergic patients is the American Latex Allergy Association, which provides helpful information and support.
Was this page helpful?Thanks for your feedback!Sign up for our Health Tip of the Day newsletter, and receive daily tips that will help you live your healthiest life.
You're in!Thank you, {{form.email}}, for signing up.
There was an error. Please try again.







